Search
Sharing Knowledge improves Knowledge... Knowledge should come at as less cost as possible.
Posts
Showing posts from March, 2016

Posted by
Varun C N
Make in India: Rotavirus Vaccine
- Get link
- Other Apps

Posted by
Varun C N
Zika infection- Updates
- Get link
- Other Apps

Posted by
Varun C N
Tarocin refurbishes β-lactam activity against MRSA
- Get link
- Other Apps

Posted by
Varun C N
India Science budget Proposal- 2016
- Get link
- Other Apps
Posted by
Varun C N
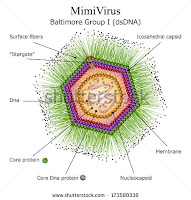
Mimi's Personal Immune System
- Get link
- Other Apps